Bipedal gait, or upright walking is the most common functional movement that we perform as human beings. The human body was designed to move athletically on two feet with upright postural design. We were designed to walk upright, to run fast, and to navigate our environment on two feet.
If your patients present with postural distortion patterns during gait, it is affecting their dynamic human potential. How your patients walk is a reflection of their posture in motion.
How your patients walk is a reflection of their posture in motion.
The Posture System is composed of four Posture Quadrants. As your patients are walking, evaluate the alignment and fluidity of each Posture Quadrant in relation to one another. Watch how your patients resist gravity while walking.
- Do they demonstrate confident upright postural design?
- Or do they have depressed and slow gait?
The gait cycle should be fluid and athletic. As one leg goes forward, the opposite arm counterbalances. As the heel strikes the floor the ground force reaction is transferred throughout the body. When the heel touches the ground it initiates the first moment of a complete gait cycle.
Are You Performing Gait Analyses in Your Practice?
Gait Analysis is an important clinical tool. It allows you to determine the patient’s posture in motion and to monitor their progression over time. Gait analysis is an objective evaluation that you can continue to monitor as the patient advances through their treatment plan.
Discover ‘step-by-step’ gait analysis protocols to determine if the patient has dynamic postural distortion patterns. Gain more certainty on how to implement gait analysis in your practice with the following tips.
How to Perform Gait Analyses
When performing gait analysis you want to follow a systematic approach. Systematizing your clinical analysis optimizes the quality of information that you see and record from the examination.
1. Patient’s Shoes Off
The first step to all gait analyses is to have the patient take their shoes off and if necessary pull up their pant legs so their feet can easily be seen. It is optimal to have the patient wears shorts. Restrictive clothing may affect their normal gait pattern.
2. Record The Patient
It is recommended to record the patient walking. There are so many things to evaluate at one time, you don’t want to miss anything. When you have the recording you can watch it multiple times, and you can watch it in slow motion.
By watching it in slow motion you can see and measure precise angles of each phase of the human gait cycle. You can also see slight abnormalities that may be overlooked by the naked eye. These slight abnormalities, if left uncorrected can lead to larger postural distortion patterns, and/or pain and injuries of the lower extremity.
3. Have The Patient Walking
For gait analysis it is considered best practices to have the patient walk on a treadmill. When they get on the treadmill allow them to select their walking speed so they are walking at a comfortable pace. If they are walking too slow or walking too fast this can impact their normal gait pattern. Allow them to self-select the gait speed. Most patients will select 3.5-4.5 speed levels on the treadmill.
If you do not have a treadmill in your office you can watch the patient walk in a long hallway or across a long room. Ensure that the space where you perform gait analyses allows adequate room for the patient to have multiple strides. You want to watch them walk for at least 3 complete strides.
4. Video Multiple Angles
When performing the video analysis with the patient on the treadmill you will take the video from the lateral and the posterior aspect (it is difficult to see from the front with a treadmill). If watching the patient walk in your office you can video their gait from the front, lateral, and posterior aspect. For best practices, ensure that the Ipad or Camera is straight, still, and shows the patients whole body for a complete analysis.
If you feel that the patient has changed their gait pattern because “they are being evaluated” then allow them to walk for a couple of minutes without analyzing them. They will be in their normal gait pattern. Then perform the analysis.
5. Fatigue Their Neurology
You can also Dual Task the patient to see their postural distortion patterns quicker and easier. Dual tasking adds stress to patient’s neurology. Because they are being dual tasked they will experience neural fatigue sooner and their postural faults will be more obvious.
Dual Tasking During Gait:
- Have them count backwards from 100 by 7s
- Have them say every other day of the week out loud in reverse order
- Have them say every other month of the year out loud
‘Step-by-Step’ Gait Analysis Summary
- Perform gait analysis using your Postural Neurology Gait Guide on all initial evaluations and follow up re-evaluations
- Have the patient take their shoes off and pull up their pant legs so you can see their feet
- For best practices video tape the gait analysis
- Utilize a treadmill if possible
- If you don’t have a treadmill, then perform gait analysis in a long room or hallway
- Treadmill Analysis
- The patient self-selects their walking speed
- Video from the lateral and posterior aspects
- If not using a treadmill, video from the lateral, posterior, and anterior aspects
- If the patient’s gait seems different because they are being analyzed, have them walk for a couple of minutes then perform the analysis
- To see the postural faults quicker and easier, use Dual Tasking to slightly stress their Posture System.
Dynamic Posture Gait Analysis
When performing Gait Analysis to see the patient’s posture in motion, you want to analyze each of the four Posture Quadrants of the Posture System. Take note of the presence of postural distortion patterns. Here is what to look for in each of the posture quadrants.
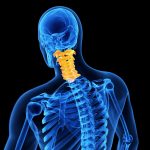
Posture Quadrant 1 (Head and Cervical Spine)
- Forward Head Posture
- Lateral Head Tilt
- Head Rotation
- Jaw Clenching
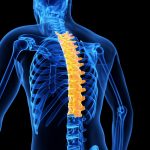
Posture Quadrant 2 (Upper Extremity, Thorax, and Thoracic Spine)
- Postural Hyperkyphosis (Flexor Dominant Posture)
- Anterior Rolling of the Shoulders
- Shoulder Unleveling
- Thumbs pointed toward the body (should be pointed forward)
- Decreased arm swing
Posture Quadrant 3 (Abdomen, Pelvis, and Lumbar Spine)
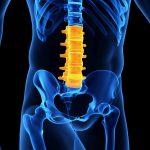
- Anterior Pelvic Tilt (Lumbar Hyperlordosis)
- Posterior Pelvic Tilt (Swayback Posture)
- Pelvic Unleveling
Posture Quadrant 4 (Lower Extremity and Feet)
- Pronation
- Supination
- Toe In Foot Flare
- Toe Out Foot Flare
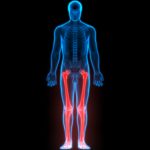 Knee Varus (Bowed Legs)
Knee Varus (Bowed Legs)- Knee Valgus (Knock Knee)
- Knee Hyperextension
For a complete understanding of Gait Analysis from a neurologic perspective, download this free guide and share it with your colleagues. In the free guide you will learn how to analyze gait from a biomechanical and a neurologic perspective. You will see how injuries and external factors impact gait patterns. You will also get a free graphic showing the human gait cycle.


Leave a Reply
You must be logged in to post a comment.